Introduction
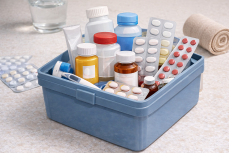
In India, medicines are easily available, and most families keep a small medicine box at home. Many people take medicines without thinking much because “it worked last time” or “someone in the family suggested it.” As a pharmacist with real experience, I see these mistakes every day at the pharmacy counter. Most people do not make these mistakes intentionally. They simply lack proper guidance. Small medicine mistakes may look harmless, but over time they can cause serious health problems like stomach damage, liver issues, kidney problems, or even medicine resistance.
Why Medicine Mistakes Are So Common in Indian Homes
In my years of experience as a pharmacist, I have noticed one thing very clearly
most medicine mistakes do not happen in hospitals.
They happen at home.
In India, we often:
- Store medicines for years
- Reuse old prescriptions
- Share tablets with family members
- Trust advice from neighbors more than professionals
People do this with good intentions, but small mistakes can slowly turn into serious health problems.
That is why awareness is more important than fear.
In this article, I will share common medicine mistakes Indians make at home, explain why they are dangerous, and guide you on how to avoid them safel
1. Taking Medicines Without Proper Advice
Many people take medicines suggested by friends, relatives, or neighbors. Painkillers, antibiotics, and cough syrups are commonly taken without consulting a doctor or pharmacist.
As a pharmacist, I often hear:
“Doctor ne pehle diya tha, isliye ab bhi le rahe hai.”
The problem is that same symptoms do not always mean the same disease. Wrong medicine or wrong dose can worsen your condition.
Real-life example from my pharmacy:
A patient reused an old antibiotic for fever.
Later, tests showed it was viral fever-antibiotics were unnecessary and harmful.
What to do instead:
- Always ask a pharmacist or doctor
- Never copy someone else’s prescription
2. Using Old Prescriptions Again and Again
Reusing old prescriptions is a very common habit in Indian homes. People keep prescriptions for years and use them whenever similar symptoms appear.
But health conditions change with time. A medicine that was safe earlier may not be safe now.
Many patients come to the pharmacy and say:
“isi bimari k liye Doctor ne last time yehi diya tha.”
But your health condition may have changed.
As a pharmacist, I always explain:
- The same symptom can have different causes
- Old medicines may no longer suit your body
- Dosage depends on age, weight, and current health
Pharmacist advice:
Never use a prescription that is more than 3–6 months old, especially for antibiotics, BP, sugar, or thyroid medicines.
3. Stopping Medicines Too Early
Many people stop medicines once they feel better. This is especially dangerous with antibiotics.
Stopping antibiotics early can:
- Increase infection again
- Cause antibiotic resistance
- Make future infections harder to treat
This mistake is very common with:
- Antibiotics
- BP medicines
- Diabetes medicines
People think:
“Ab theek ho gaya, medicine band.”
But stopping early can:
- Bring the illness back
- Make bacteria resistant
- Cause BP or sugar to rise silently
I always tell patients:
“Complete the full course, even if you feel fine.” If a doctor says “5 days,” it means 5 full days, not “till relief.”
4.Taking Medicines at the Wrong Time
Some medicines should be taken:
- Before food
- After food
- At fixed times
Many people take medicines randomly, skip doses, or double the dose if they forget.Taking them at the wrong time can cause stomach pain or make the medicine useless.That’s why we should follow simple rules below:
Simple rule:
- Never double a dose
- Never misse a dose
- If miss a dose always counsult a doctor of ask this to your pharmacist.
- Ask your pharmacist about correct timing
5. Mixing Medicines Without Knowing Interactions
Taking multiple medicines together without knowledge can be risky.Many pepole in India specially in rural area they are doing this kind of mistakes regularly,and they dont even think about the interactions .
Common mistakes:
- Painkillers with alcohol
- Two cough syrups together
- Herbal medicines with allopathic medicines
Warning signs of interaction:
- Dizziness
- Excess sleep
- Stomach pain
- Vomiting
Always inform your pharmacist or doctor about :
- All medicines you take
- Ayurvedic / herbal products
- Vitamins and supplements
They don’t realize medicines can react with each other.
6.Storing Medicines Incorrectly at Home
In many Indian homes, medicines are stored:
- In kitchen cabinets
- Near gas stove
- Inside bathroom shelves
- In bathrooms
- Near kitchen heat
- Without covers
Heat and moisture can damage medicines.
Heat and moisture can:
- Reduce medicine strength
- Spoil syrups
- Damage insulin and eye drops
Correct storage tips:
- Store in a cool, dry place
- Keep away from sunlight
- Refrigerate only if mentioned
- Store medicines in a cool, dry place
- Keep insulin in refrigerator (not freezer)
- Never store medicines near sunlight
7. Using Expired Medicines
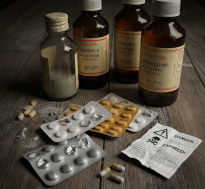
Using expired medicines is a topic that comes up often in the pharmacy world. While many people think of expiration dates as “suggestions,” as a pharmacist, you likely know they are critical for guaranteeing that a patient receives the exact dose and safety profile the manufacturer intended.
Here is a breakdown of what happens when a medication expires:
Loss of Potency (The Most Common Outcome)
Over time, the active ingredients in medicine break down due to exposure to light, heat, and moisture.
- Reduced Effectiveness: The drug simply becomes weaker. For a headache, this might just mean slower relief.
- Critical Risk: For life-saving medications, a drop in potency is dangerous. If an EpiPen or Nitroglycerin tablet has lost 20% of its strength, it may fail to stop an allergic reaction or a heart attack Risk of Bacterial Growth
This is particularly a concern for liquid medications, such as:
- Eye Drops: Preservatives break down over time, allowing bacteria to grow. Using expired drops can lead to serious eye infections or irritation.
- Cough Syrups & Suspensions: These formulations are more prone to contamination once the seal is broken and the date has passed.
Chemical Changes & Toxicity
While it is rare for a medicine to become “poisonous” immediately, chemical degradation can occur:
- Tetracycline: This is the most cited historical example where expired versions were linked to a rare form of kidney damage (Fanconi syndrome), though modern manufacturing has reduced this risk.
- Unknown Byproducts: As chemicals break down, they can turn into different substances that may cause unexpected side effects or allergic reactions.
Antibiotic Resistance
Taking expired antibiotics is a significant public health concern. If the antibiotic is sub-potent (too weak), it won’t kill all the bacteria. The surviving bacteria can then adapt, leading to antibiotic resistance, making future infections much harder to treat.
Medications You Should NEVER Use Expired:
| Medication Type | Risk |
| Insulin | Becomes unstable; leads to poor blood sugar control. |
| Epinephrine (EpiPen) | May not be strong enough to stop anaphylaxis. |
| Nitroglycerin | Loses potency very quickly once the bottle is opened. |
| Liquid Antibiotics | Degrade much faster than tablets and can grow bacteria. |
| Oral Contraceptives | Even a slight loss in hormone potency can lead to unplanned pregnancy. |
Pharmacist tip:
Never use syrups or eye drops after expiry or after long opening.
8.Giving Adult Medicines to Children

Giving adult medications to children is a common mistake, but it can be very dangerous. Here is a simple breakdown of why you should avoid it and how to keep your children safe.
Why it’s Risky
Many parents think, “If I just give half the tablet, it will be fine.” Unfortunately, it doesn’t work that way.
- Children are not “Small Adults”: A child’s body (especially the liver and kidneys) is still developing. They process medicine differently than adults do.
- Wrong Dosage: Even a small “adult” dose can be an overdose for a child, leading to serious side effects or toxicity.
- Harmful Ingredients: Some common adult medicines, like Aspirin, can cause rare but life-threatening conditions (like Reye’s Syndrome) in children.
Best Practices for Indian Parents
- Check the Label: Always look for “Pediatric” or “For Children” on the packaging.
- Use the Right Tools: Never use a regular kitchen spoon (charach) to give syrup. Use the calibrated dropper or measuring cap that comes with the bottle to ensure the exact ml is given.
- Weight vs. Age: In India, doctors often prescribe medicine based on the child’s weight, not just their age. Always follow your pediatrician’s specific advice.
- Avoid “Double-Dosing”: Many cold and cough syrups contain the same ingredients (like Paracetamol). Giving two different syrups might accidentally double the dose.
Golden Rule: If the medicine doesn’t have a specific dosage for a child’s age or weight on the cover, do not give it. Always call your doctor first.
9. Not Reading Medicine Labels
Medicine labels contain important information like:
- Dosage
- Warnings
- Storage instructions
Ignoring labels increases risk.
10. Avoiding Pharmacist Consultation

Many people hesitate to ask pharmacists questions.
But pharmacists are trained medicine experts.
My advice as a pharmacist:
Ask questions freely. It can protect your health.
How to Avoid These Mistakes
✔ Always consult a doctor before starting or stopping medicines
✔ Ask your pharmacist if you are unsure
✔ Read labels carefully
✔ Follow correct dosage and timing
✔ Keep a list of medicines you take
✔ Educate family members
Final Words From a Pharmacist
Medicines are meant to heal, not harm.
But only when used correctly.
I have seen patients suffer—not because medicines were bad,
but because they were used the wrong way.
A little awareness can prevent:
- Side effects
- Hospital visits
- Long-term damage
Safe medicine use starts at home.
Medicines are meant to heal, but only when used correctly.
Most medicine-related problems happen due to lack of awareness, not bad intention.
As a pharmacist, my message is simple:
When in doubt, always ask your pharmacist or doctor.
Safe medicine use can protect you and your family from serious health problems.
If you are confused, don’t Google blindly—
ask a professional. It can save your health.
Frequently Asked Questions
Is it safe to take medicines without consulting a doctor?
No. Even common medicines can cause side effects or interactions. As a pharmacist, I always advise consulting a doctor or pharmacist before taking any medicine.
Can I reuse an old prescription if symptoms are same?
No. Your health condition may change. Old prescriptions should not be reused without medical advice
Are expired medicines dangerous?
Yes. Expired medicines may not work properly and can cause harm.
Can herbal and allopathic medicines be taken together?
Not always. Some herbal products interact with modern medicines. Always inform your doctor or pharmacist.
How should medicines be stored at home?
Store medicines in a cool, dry place away from sunlight, heat, and moisture.
Stay Safe. Stay Informed.
If you found this article helpful,
bookmark this page and share it with your family.
As a pharmacist, my goal is simple:
to help Indian families use medicines safely and wisely.
Follow SafeMedsSkinGuide for trusted medicine & skin care advice.


Pingback: Antibiotics Without Prescription: A Dangerous Habit...